As some states reopen, others pause reopening, and more consider shutting down again, figuring out what is and isn’t safe to do can feel like a nationwide game of “red light, green light.” In a recent Kaiser Family Foundation poll, 52 percent of adults reported that they or a family member had skipped a medical appointment because of COVID-19. Sadly, the most common appointment skipped was for dental care.
In North Carolina, many dental offices are still closed, and others are only open for emergency services or are limiting services as they reopen. If your dental office is open for full services, you still might choose to stay home if a family member is immunocompromised, or if you are concerned about North Carolina’s rising case count, which is regularly topping 1,000 new confirmed cases daily.
Regardless of the reason, if you or a loved one are staying home and have missed an appointment—or even if you have seen a dentist or will see one soon—here are some steps we all can take for better oral care at home.
Use Fluoride Toothpaste AND Mouth Rinse
While brushing your teeth alone is important, fluoride actually strengthens your enamel and in some cases can reverse early signs of tooth decay. Fluoride toothpaste can be used at all ages, but it is important to use the right amount.
Mind Your Peas and Q’s
Fluoride toothpaste can be used as soon as a child’s primary teeth have started erupting from the gums. Before age three, just use a smear of toothpaste, no more than the size of a grain o rice. Start using a “pea at three”—a pea-sized amount of fluoride toothpaste for children and adults ages 3 and up.
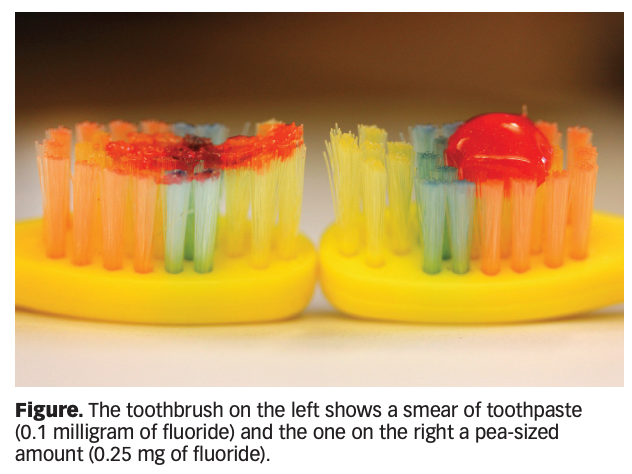
Source: American Dental Association
Remember that less is more. You really don’t need the long squirt of toothpaste covering the entire brush you may see on commercials.
Know the Basics of Good Brushing
The saying doesn’t go “close only counts in horseshoes and brushing your teeth.” Brush for two minutes to ensure that you hit every single tooth, even those back molars. Two minutes may feel like a long time, but it is necessary to properly brush all sides of all your teeth.
While brushing, makes you are you are using circular motions. Brushing with a sawing motion can actually harm your teeth by increasing abrasive removal of your enamel and potentially damaging your gums. You should only apply mild pressure to your brush, about the same amount of pressure you would use to write with a pencil. It might feel like you aren’t cleaning hard enough if you use less pressure, but that’s just another reason why the full two minutes is so important!
Last, but not least, don’t forget about your tongue. Bacteria and other germs can build up on your tongue and can contribute to tooth decay, gum disease, and bad breath. Brushing your tongue is an important part of maintaining good oral health.
Change your Brush Regularly

When your brush becomes frayed, its time to replace it.
Most dentists recommend changing your brush every three months or when the bristles become worn down.
Floss Daily
Brushing thoroughly can clean three sides of your teeth, but brushing alone can’t remove plaque or bacteria in between your teeth. Adding floss to your routine is an extra layer of protection from cavities, tooth decay, and gum disease.
Check your Mouth Regularly for Signs of Oral Cancer
Oropharyngeal cancers kill one person every hour in the U.S. Fortunately, early detection significantly increases survivability. Self-exams for oral cancer warning signs are quick and easy, and they are an important component of a healthy oral routine.
Check out our recent graphic about oral cancer and HPV for self-exam guidelines.
Click here for a full PDF to access any hyperlinks above.
Know How Your Food Affects Your Teeth
What we eat can seriously impact our oral health, even with good brushing habits.


To learn more and get involved, be sure to sign up for NCOHC news.
NCOHC is a program of the Foundation for Health Leadership & Innovation. For more information and to stay up to date, subscribe to the NCOHC newsletter. If you are interested in becoming an NCOHC member, you can also fill out our membership form. It’s free!























